So much has been written about the ageing of our population and the impending retirement of the ‘baby boom’ generation that you would think we were awash in elderly. You may have seen headlines like, ‘The Grey Tsunami’. The economic principles of supply and demand state that if there are lots of older people (demand) then care homes, nursing homes and domiciliary care agencies (supply) should be operating at capacity and even expanding to meet the growing demand.
Yet, many operators and managers still report poor occupancy, voids or available capacity to take on extra clients. As we will see, these anecdotal reports are borne out in the facts that care home, nursing home and housing with care supply has been shrinking.
This paradox begs a simple question. If there are so many older people, why isn’t the demand greater? Why aren’t care homes, nursing homes and other care provision full, with more capacity being added every day?
Many operators and managers point to the influence (even interference) of intermediaries such as regulators and local authorities to explain why they aren’t full and why they need to close homes or remove capacity from the system. While the impact of these intermediaries is undeniable, this explanation isn’t at all complete.
Demographic Facts
The demographics of ageing are not as simple as has been portrayed in the popular press, by advocacy groups in the sector or by policymakers. The population is growing gradually older, however those accessing care services has been shrinking. The ‘market’ (the number of older people requiring care and support) is declining. In a declining market, the supply (the capacity of services for this market) also declines.
Demographic Dip
If we look more closely at the live births in the England and Wales we can see this ‘demographic dip’ in Figure 1.
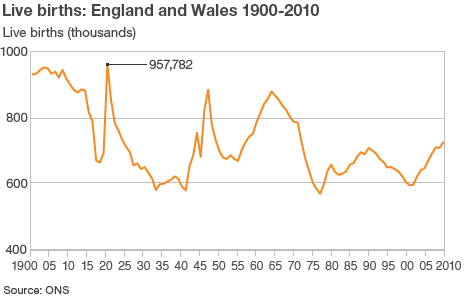
The live births peaked at approximately 960,000 in 1920. (Those born in 1920 and who survive, reached 75 in 1996, and 85 in 2006.) The birthrate then went on a steep decline until approximately 1942. Of course this ‘demographic dip’ corresponds with periods of war, great economic and geopolitical instability. The next ‘peak’ in birth rates is in 1946 at approximately 850,000 births, and then there is another decline and trough (corresponding with the postwar recession) until 1955. Of course, these peaks and troughs must be reflected as the population ages.
Demand for care services and housing with care is greatest at approximately age 75 to 85. There is certainly demand among the younger population and some demand after 85, but the average age of relocation to care settings, and the height of service use occurs between the ages of 84 and 87. This means that in 2014, those accessing care services were born between 1926 and 1929
The population of those likely to require care services has been declining, will continue to decline and will not rebound until 2025.
These demographics will have a deep, protracted impact on the demand for services. It is this ‘demographic dip’ in combination with symptoms of the recent ‘great contraction’ (think recession on steroids) which are depressing demand.
There has been an extraordinary array of reports and projections about a rapid growth in the number of older people. These make great bylines in the popular press. Most of these reports rely upon the ‘rate of change’ rather than the more granular number of people, and often project the change from 2010 to 2030 or even 2050. For infrastructure and strategic planning purposes such projections are extraordinarily important, but if you’re trying to run a care home in Yorkshire, or domiciliary care agency in Surrey, if your market is shrinking today, next year and the year after, you may not survive to 2030.
The Dilnot Report shows the rate of growth amongst older people and not ‘the number’ .
Teh rate of growht depicts a dramatic charge, and one can find many of these in many reports and documents. The truly important thing today, and in the near term isn’t the percentage difference in older people from 2010 to 2030 as much as the numeric change between now and 2030. The estimated total 85+ population in the UK will grow from approximately 1.8 million to 3.6 million from 2010 to 2035. This is a dramatic rate of growth over this period of time, but the overall number is relatively small, and in the near term, from 2014 to 2020, we are faced with a flat or declining market.
The supply
This demographic dip and resulting decline in demand is reflected in the number of available residential and nursing care beds reported by Laing & Buisson and others.
The decline in total utilisation from 472,000 in 1990 to 418,000 on 2010 (decrease of 11.5 %) represents the type of contraction in supply to be expected in a declining market. The decline in the available supply cannot be explained merely as the result of policy changes or intermediaries; this is supply and demand at work in the nursing and care sector.
What about lifespan?
Having presented this challenging, contrarian scenario in several national and international conferences, some of the arguments against the downward drag of the demographic dip on the care market have been offered up.
Many would argue that the increasing life expectancy and declining mortality since 1920 would offset the effects of declining birth rates. The arithmetic of this, however, simply doesn’t work because of the scale of the decline; live births declined by over 360,000 between 1920 and 1935. Life expectancy would have to have increase by a factor of 2.5 to 3 (more than double) among those 80 years of age or older to achieve survival rates that would compensate for the decline in live births.[2] Increased life expectancy and decreased mortality, while offsetting this decline, cannot adjust for the size of the demographic dip.
What about chronic diseases?
With a society which is gradually ageing and enjoying improved survival and lower mortality, some argue that the chronic diseases of ageing (orthopedic, neurological and cardiovascular) will compensate for the demographic dip by increasing the demand for services among the declining older population. Prevalence of Alzheimer’s disease and related conditions among the population seems to be increasing. However because these illnesses and diseases are primarily late onset, the incidence results in burden, therefore demand, mostly as the population ages.
What about acceptance?
One way to compensate for a declining market demand is to increase the acceptance or penetration of the product or service. It is a fundamental truth, however that in our societies, care home and nursing home use can be seen as negative. Negative press, ageing stock and public squabbles have further tarnished the perception of care services. Try as we might, this will be hard to change.
What to do?
In a free and open market system, supply would contract to meet the available demand. Furthermore as the consumers’ needs and desires change, the suppliers would adapt and modified the product or service. It is unlikely that this will occur easily and without some significant convulsions. After all, entering the care market as a provider is not, nor should it be, easy so market exits will be difficult and potentially traumatic.
From a public policy and budgeting point of view, it makes little sense, in my opinion, to demand more resources now, when the market is declining. Preparation must be made for the inevitable increase in demand that will result when the oldest baby boomers reach the age of high consumption around 85. This is in approximately 15 years’ time. In a collaborative environment, this should offer sufficient time to consider the most beneficial and least costly options. For example, assistive technology to improve the safety and surveillance of the health of any population. The baby boom population and those who come later will expect care providers to have technology sophistication.
For operators and managers, the goal is to survive the next decade or so. There are four demonstrated strategies to survive a declining market.
1. Improve customer/consumer loyalty. In a declining market, increased market share comes at a very high cost, therefore, retaining existing customers and consumers is imperative. Loyalty depends upon effective service error recovery and most managers are not accustomed to applying these principles in their daily operations.
2. Increase efficiency. This does not mean cutting staff, as is commonly understood. Higher levels of output for the current inputs is the principal of achieving higher efficiency. The principles of continuous quality improvement, LEAN and Six Sigma management techniques must be imported to the sector.
3. Innovation. Capital investment in innovations, such as technology, which have a measurable impact on improving efficiency, as well as increasing customer loyalty will allow some operators to survive – others will be left behind.
4. Differentiate. Novel programmes, such as innovative ways of caring for people with dementia, new technologies which allow staff to spend more time with residents and families, will offer providers marketing and public relations opportunities to demonstrate to potential clients how they differ from their competitors.
Survival
Surviving the demographic dip will be a challenge for the sector. Being realistic about the imminent changes and responding effectively will allow certain providers to survive and continue serving older people, as well as their families.
Irving L. Stackpole RRT, MEd
