Date: 2nd November 2021
To watch the recording click here
Register to download the webinar presentation.
Transcript
Designing the Future of Long Term Care
Facilitated by Irving Stackpole, with Susan Ryan from The Green House Project and Jamie Timoteo from Plante Moran.
[Irving]
We have seen quite a few changes in long term care. We’re going to talk briefly about how we got to where we are in long term care and what we need to do to move forward. And we have two important guests in this program today to add to this discussion in several important dimensions.
First of all, the question is how did how did we get here? We got to the situation in the United States with regards to congregate long term care through a not very complicated channel. The first is that there used to be poor houses and those poor houses became nursing homes. Those nursing home buildings, in the United States most of which were built in the mid 60s to the mid to late 70s, most of those facilities got old – along the way we stopped investing in those facilities and we stopped building new ones for reasons that I can discuss on another program. These buildings, these long term care facilities, are pretty much filled up with people. One of the challenges is that health care professionals resisted the idea of working there. Unfortunately, state and federal regulations came along that required nursing home managers to hire more and more people, and we restricted payment in the United States to these nursing centers. We reimbursed them below their actual costs, and instead of cutting back on what was required of them, we basically told them to do more. This was a recipe for difficulty, and certainly not a good recipe for successful formula for a long term care.
Then COVID 19 hit. The structures and design in long term care and the built environments in long term care have progressively deteriorated and are in a very difficult situation. The article that is on the screen right now was recently published in New Yorker magazine, and it out-and-out said that the American nursing home is a design failure. As I said earlier, most were built in the 60s and early 70s and were modeled on hospitals. They pretty much used the same blueprint of hospitals; where the space is optimized not for the experience of the residents but for the efficiency of the providers.
Assisted living came along in the late 80s, early 90s and it offered a very updated version for longer term, chronically ill individuals. Assisted living siphoned off a lot of the consumers from nursing centers, consumers which historically paid private rates to nursing centers for their long term residents. Once assisted living siphoned off a lot of those private patients, and for reasons that are pretty apparent to those of us who have been in both in assisted living residents versus a skilled nursing center in the United States, since then (the 1990s) there’s been little or no reinvestment in the built infrastructure in congregate long term care.
The capitalization, the investments, have been fundamentally extractive. There has been money taken out of the system in the form of real estate transactions or in the forms of sale leaseback transactions. The federal government, meanwhile, withdrew fiscal support for long term care long ago. There is only a very small proportion, about 11 percent of the payments for congregate long term care, that are sourced through the federal government. The result, I hope this isn’t overstating the case too badly, the result is: yuck.
The question is: would you like to stay at a Hilton or a Marriott that hadn’t been renovated for 40 50 years? Probably not. Apparently not very many other people want to either. The question is then: to redesign this future, which we should all recognize is needed, what do we need? First of all, we need more variety. The cookie cutter approach to building the built environment in long term care just isn’t going to cut it. It isn’t going to cut it for baby boomers, and it certainly didn’t cut it when it came to COVID 19. We need large infrastructure like college dormitories with attractive common spaces. We need medium size infrastructure like the current, almost cookie cutter approach that’s been taken by dominant players / dominant organizations in that segment. We need medium-sized assisted living as well, but we also need small models like the greenhouse model and even McMansions. Sometimes these tie together in naturally occurring retirement communities – I think the Golden Girls is a good example. The important thing is that real estate undergirds the sector, and whether the fundamental investment is through equity investment or debt, the current situation is problematic.
How do we redesign the built infrastructure with the current financing models, not necessarily the reimbursement models, but the capitalization models? That’s one of just one of the reasons why we’ve invited these two distinguished panelists to join us today. Access to capital is an issue. We need a good, rational model for how to accomplish that, and we have two nationally-recognized presenters here to help us walk through these issues.
[Jamie]
Irving, thanks for for setting the stage there, and I appreciate everybody tuning in today and I echo Irving’s sentiment about sharing your time with us. My name is Jamie Tomateo, I lead our pre-development services for Plante Moran Living Forward. Our practice focuses entirely on senior living development consulting. This trend that we’re seeing in the nursing home industry with some of the issues that Irving just outlined is something that we deal with on an everyday basis with the clients that we work with daily.
What I wanted to do just kind of set the stage first is I’m going to talk to a couple of trends that we’re seeing in the nursing home industry, and I’m also going to talk through a little bit on the margins that we see in the existing environment out there for skilled nursing. Susan is going to come in afterward and give us background about the Greenhouse model and how those buildings operate and function, and then I’m going to wrap us up on financially how we’ve had some of those models work for our clients and how we’ve approached them with organizations.
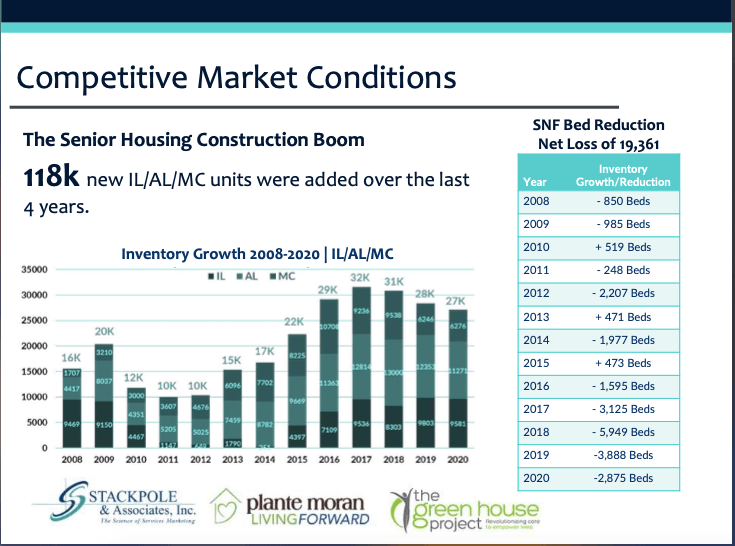
The first piece I wanted to run through is over the last decade, what’s been going on and new construction that’s happening in the senior living industry kind of in total. What we have here is the bar chart representing new units that have been added specifically for independent, assisted and memory care. You can see kind of 2008-09 going into the recession there was a dip or a little bit of a lull in new units that were added in the largest 31 markets across the U.S.. Since then we’ve had a consistent uptick every single year, essentially through 2018, and we still are really strong in 2019 and in 2020 – during COVID, we still added about 27,000 new units of housing (independent, assisted and memory care). But what we’re seeing kind of across the country now, I don’t think it’s that much of a surprise, is every year that we’re adding new units of more housing, the number of beds on the skilled nursing side has been reduced.
In that chart on the right of our screen here is: outlining the number of beds that were taken offline and reduced in circulation across the country. If you kind of look at it from 2008 to 2020, every single year had a reduction except for three years. There’s really kind of a trend that we’re seeing across the industry. Rvery engagement that we have has some form of skilled nursing repositioning and in a sense, the downsizing that’s happening. A lot of that goes to the attractiveness of the product that Irving kind of touched on at the beginning here. What I wanted to share is: the utilization that we’re noticing across the United States. I gave a comparison just on the state of Ohio as well on how many nursing home beds are being utilized in the nation and in the state of Ohio. What I’m showing on this screen is the number of nursing home residents that reside in a skilled nursing setting. It’s really kind of that ‘top’ number – if I looked in 2020, nationally we had a little less than 1.3 million people living in a skilled nursing setting. We take that as a percentage of the population 65 and older. If you look at the trend over the last decade, every year we’ve seen a steady and slow decline. So there are less and less people who are age-qualified (theoretically that would that would be moving into a skilled nursing setting). A lot of this can be attributed obviously to the number of housing units that were being added, showed on that previous slide, but another piece could be added that the government is pushing individuals to this better product that’s being offered out there.
So if people can afford to live in a better living environment, maybe in assisted living and receive almost the same care in some settings, they’re choosing to pay for that until they absolutely need to. Neither truly need skilled care or they run out of funds and may have to qualify for Medicaid reimbursement. The trend in the skilled nursing environment has been, historically over the last decade, really trending negatively.
Nationally, and I have this map that’s representing different regions here because I want to show you two slides in a row that talk about the margins that we see in a skilled nursing environment, these margins are specific to the existing environment for all skilled nursing across the country. We show it both nationally as well as by each of the regions that are that are colored on this map. One of the things I wanted to make sure is abundantly clear is: you hear a lot of times people talk about the Greenhouse project as a great option for skilled nursing, but we can’t get the numbers to financially work. One of the things that we always try to have our clients level set and come back to is: if you were to look at the existing environment in a skilled nursing setting and the profitability for many of those organizations, many times those existing products that are functioning out there are also not profitable. Therefore, the argument that a Greenhouse project may not financially work really may depend truly on how you plan to operate that environment.
What I wanted to also share is just nationally, some of the trends. The first ratio here that we’re looking at is our EBITDA margin. Essentially, our earnings before interest, depreciation and amortization. Here is what it is for the different regions that I had shown in that previous slide. Nationally, the average for our EBIT margin is is just a little less than 10% for the existing skilled nursing environment. You can see across the country it kind of varies depending on what region you fall in. One of the things I do want to point out that these numbers do represent 2018 results – so we’ve looked at this well before COVID started coming into play because we wanted to have the where were you before COVID benchmark set. I think if we started looking at this with COVID numbers factored in here, you have an even more grim picture, potentially.
In this last slide that I wanted to point out what our net margin looks like. This factors in your interest and your depreciation and amortization. When you add those components in there, you kind of are really looking at your bottom line net income for an organization. Skilled nursing homes, for the most part, essentially broke dead even or lost some money. Nationally, it was about a 0.21% margin for for the existing skilled nursing environment that we have out there. A lot of the organizations that are offering skilled product are making the conscious decision to say the existing product that we offer does not work, should we explore other options? And if we do explore those, how how do we get them to work? Some organizations I know are shifting, saying “I’m going to offer more of a housing product, so I’m going to add more independent, more assisted, more memory care, and I’m going to just downsize the number of nursing home beds I offer to to to the residents in our community.” Others are saying they still want to maintain the number of nursing home beds, and so they’re are looking at other avenues and ways to do that and to make them attractive and viable long term into the future. When we dive into that, I want to hand it over to Susan to kind of talk about some of the cultural impact in the staffing models that we’re seeing in the Greenhouse Project.
[Susan]
Let’s talk a little bit about the Greenhouse model. What I first want to do is to ask you to think Irving for setting such an incredible context: I appreciated what you said about how we got to nursing homes that are modeled after traditional hospitals. The other thing that Irving said that I really resonated with was that the structures were really created for efficiency, and not really thinking about the people that would be living inside them. Also the call for more variety – I couldn’t echo that more. Moving to Jamie, some of the comments you made: you talked about downsizing, the lower utilization, and I think for me, I would say there’s not a one size fits all (number one). Rather than downsize, let’s call it “right size”, and let’s figure out what we need to build and what we need to do, given some of the realities we’re in right now in a COVID environment.
First, let me unpack what the Greenhouse model is. I’m always amazed at how many people still think Greenhouse might refer to some sort of green environmental initiative or a literal green house, so let me talk more about what the Greenhouse model is. I would tell you, as a nurse of greater than 40 years working in home care settings and long term care settings, this is a radical paradigm shift – that it’s not just the physical environment that we see, but it really is a comprehensive transformation of also the philosophical culture and the organizational structure. I think of it as a three legged stool; you really need all three legs, each are important – you don’t want one larger than the other, but they’re really equally important to really creating and being a part of that radical paradigm shift. The other thing, as someone who has been a part of culture change initiatives as long as I’ve been working in long term care, it’s one thing to implement change and another thing to sustain it. For me, the Greenhouse model is really about a radical paradigm shift that’s comprehensive in nature and it’s really about sustaining change.
Let’s unpack it by our Core Values. That physical environment, when you think about what is the right structure? Well, we don’t want home-like, we want real homes. So that physical environment “real home” is the core value that refers to Greenhouse. What does it take to get us there, to have a real home? First of all, we believe that it should be small – no more than 10 or 12 people living in that setting, really creating more of that familial setting. In addition to that, you’ll see a heart at the top left hand corner here. At John Knox Village in Pompano Beach, Florida – that’s the heart of their living room, if you will. You can see the kitchen on the other side of that fireplace. In addition to that, privacy is important. We went private rooms with private baths, each having their own private shower within their bathroom there. Last but not least, open kitchens with meals prepared. We’ve decentralized apartments such that every home has its own kitchen, its own ability to do the laundry and its ability to do housekeeping there. It’s therefore autonomously functioning – that’s a real home. I don’t share those things with my neighbors, and we don’t think elder s should share it with their neighbors as well. One of my favorites is access to outside. I remember during the pandemic how important it was to be able to get outside and to really experience the opportunity to do those things that are more normal, which is a perfect segway into that second core value, which is: meaningful life.
It’s not just about person-centered care, where care is centered on who I am, but it’s about a deep, knowing relationship, rich person directed living. The better I know who a person is and I’m able to engage with that person, the better I’m able to help them with a meaningful and a purposeful life. A meaningful life means there’s a degree of autonomy and control in what I’m able to do. All these pictures that you have on your screen are elders during the pandemic that we’re able to experience a meaningful and purposeful life. When you contrast these with those that were taken during lockdown, everyone confined to their rooms, a semi-private room at that, having meals delivered to their rooms. So rather rather than thinking about mitigating the spread of the infection primarily, this is also promoting health and well-being, even during a pandemic. Not just the structural physical environment of a real home, but really the meaningful life that occurs in there – and it’s purposeful engagement.
You can see a couple at the top here who are celebrating a milestone anniversary honoring the natural rhythms, what’s important to a person, what’s important to them to really help them to experience a meaningful day and the real need to be socially connected. As humans, we are hard-wired to be in relationships with one another, so you can see relationships happening in each of those pictures (an integral part of our core value meaningful life).
There’s our access to outside. I love this, there’s actually a story to the gentleman that’s barbecuing on the left. This was in Tupelo, Mississippi, where barbecue is pretty darn important to them in Tupelo. So instead of a barbecue, they had what they called a quaran-cue. This is a direct care worker who’s fixing something on a grill and an elder who’s out there supervising. They are physically distanced but able to provide commentary to what he’s grilling, and on the right – I can’t tell you how many gardens were grown during the pandemic. An opportunity for elders to get outside and experience that sense of normalcy that is really a part of living and meaningful and purposeful life. Gardening activities were huge during the pandemic.
Last but not least, the third leg of the stool to me is one of the most vital and probably one of the most overlooked in many culture change initiatives. That is: how do we create an empowered workforce and how do we really utilize those that are working closest to the elders? Really getting them into consistent teams, dedicated staffing, and really embracing a coaching culture? I’ll say a little bit more about that in a bit, but having them work as a versatile worker, or you might know it as a universal worker, when you empower those that are working closest to the elder and you really support them and hold them accountable and equip them to do their job, it’s amazing what happens. A universal worker / versatile worker is somebody that does not only the care provides and needs the care needs of an individual, but that person does things like the cooking, the laundry, the housekeeping. In this case, in one of the images, you’ll see somebody who is actually doing the cooking in the house but really equipping them to be household managers. Making sure they are in those consistent assignments so that they’re able to know elders as an individual and they’re able to see what is it take for each person to be able to live his or her meaningful life. I can’t say enough about the function of leadership to make that happen.
As Irving said in his slide, “and then along came COVID”, and how did that rock our worlds? I was looking at 2020, maybe like some of you, thinking, “this is the year we’re into a new decade, this is the moment where there’s going to be great things that will happen.” Little did we know that we were going to be hit by a deadly virus affectionately (or not so affectionately known) as Covid-19. I was emailing with a friend recently, and he shared this excerpt from an interview that was done on NPR. This was an interview that was really talking about, as Irving talked about, the structures that really fueled the flame, if you will, of Covid-19. The interview was with Ed Yong, who is a science writer for The Atlantic. I’m not going to read it verbatim but I hope you will read it. A couple of things to point out to you (about it): first of all, the fact that this interviewer is referring to nursing homes along with prisons and talking about them as “cauldrons” and a “structural sickness” – this certainly builds upon what Irving has said. To put nursing homes alongside another institution where people are often warehoused, and those would be prisons. It’s interesting that the interviewer is really getting into the structural issues and the sickness of our structures, but I love Ed Young’s response. He definitely agrees with the fact that, yes, they they are structurally sick and they are cauldrons. They are definitely fueling the flame. He then talks about what I’ll call the devaluation of elders, those that are living in our traditional nursing homes. The marginalization that has occurred, and you’ll see the marginalizing referenced there, to really talk about it as truly shameful. That, why are we doing this? Some would argue it’s because of some of our aging stigmas and the stereotypes and the devaluation that is occurring as a result, and that’s why we have some of our structural sicknesses. That’s why COVID, when it went through nursing homes, created the damage that it did.
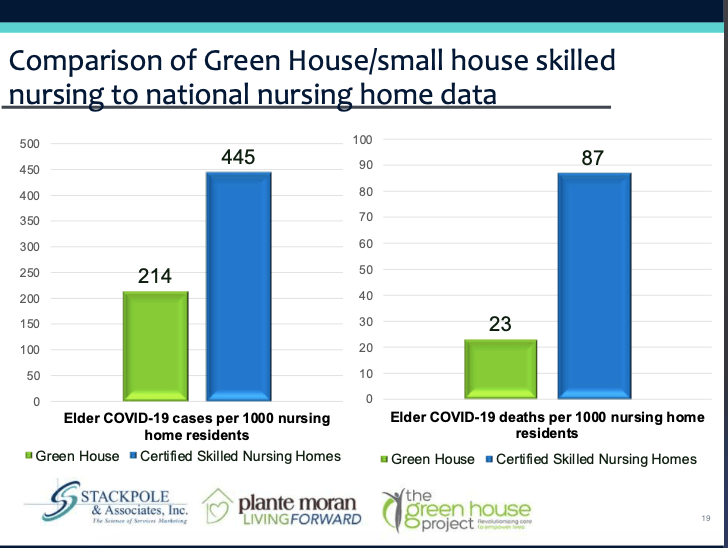
We began collecting data between among our Greenhouse homes and then comparing it to their traditional counterparts. Actually, we are continuing to collect our data. Each month we work with a researcher from the University of North Carolina, and we were utilizing a methodology that was very similar to what the CDC and CMS reporting had set up, so they weren’t being duplicative to what they were doing there.
This is just the raw data from January through December of 2020. You can see that COVID cases on the left hand side, green of course is for Greenhouse: 214 COVID cases per 1,000 nursing home residents compared to 445 per 1,000 in the traditional nursing home. On the right hand side, you will see we looked at mortality rates and per one thousand nursing home residents: 23 in Greenhouse compared to the 87 in traditional nursing homes. There was research that was published in JAMDA, and I know I sent Romilly our PDF of that research; if you’re interested in drilling down and really going down to see where our Greenhouse homes located, how did they compare to nursing homes, less than 50 beds and nursing homes in the same geography to greater than 50 beds, we’d be happy to share that with you.
Here’s the other thing, speaking to the lower utilization among nursing homes. I loved Irving’s comment at the beginning, he said, “would any of us want to stay in a Hilton that hasn’t been renovated for 40 or 50 years?” Consumer choice. When you look at occupancy rates in Green households pre-COVID (Greenhouses on the left traditional and the national average is on the right) pre-COVID we were about 97%. During COVID, it dropped to 90%. But look at the national average: pre-COVID, they’re at 83% and during COVID, down to 71%.
The greenhouse difference: we every year collect data from our organizations. In May, we looked back at 2020 to take a look at occupancy. We also looked at staff turnover and we looked at operating costs. The data you see on the right for Greenhouse is all 2020 averages across Greenhouse homes from the data we collected. It’s 2020, representing a COVID year for Greenhouse homes. The data we were able to compare it to was actually pre-COVID data. So to Jamie’s point, he was talking about some data that he had, and he said this is actually pre-COVID, this shows it it’s only gotten worse with COVID. I think pretty interesting. Obviously, staff turnover was a huge issue no matter where you were, but you can see how much better it was on the Greenhouse side of things. I love the operating costs. Pre-COVID versus traditional: we’re looking at about $276 a day on the traditional side on average and Greenhouse homes average $261 per day (also taking into account COVID expenditures).
How do you make this work? Is the question that always gets asked. I would say there’s a lot that has to do about empowering your workforce and really building a culture where people matter and really resourcing your workforce to make the model work. You can’t have jump, you’ve got to fully commit. Empowerment is as much a function of leadership and really, leaders that fully embrace the model and embrace what needs to happen by way of staffing succeed. Really thinking about what is a coaching culture? How do I share power? How do I share decision making with those that are in each of those homes so that I’m resourcing them to make wise good decisions that have impact on your cost and obviously satisfaction when your elders? It’s about leaders that will fully empower the team education and equipping this group with the core competencies. If you’re asking them to cOOK, you need a strong culinary program and making sure that they’ve got what they need to make it work. What is that communication? What is it looking like so that we’re disseminating information and making sure each team member has what they need to be successful is really owning the role and the responsibilities? How will we get the job done? What does it look like and how do we share responsibilities, share tasks that we really understand our roles?
Last but not least is making sure that self-managed work team has the necessary support to be successful and leaders are holding them accountable to doing their job well. Let’s drill down a little bit and look at the number of FTEs:
This is contemplating Greenhouse homes, probably 10 elder homes and 6 homes so 60 elders total. In a traditional facility that would be home to 60 elders, you can see the cost shifting that is essential to making it work. The Green Line obviously is Green House, and you can see far more CNAs, you have more LPNs and RNs – this is that direct care time that is going in to support those working closest to the elder. Then it’s the shifting that is occurred: administrative and clinical support, which can be costly care or costly in terms of wages, you have more on the traditional side, less on Greenhouse side. Obviously, your dietary, foodservice, laundry, housekeeping, all of that is way down in Greenhouse and way up on the traditional side because of that cost-shifting that we’ve done.
There was some research that was done in 2009-10, where they were really taking a look at the total time, the hours per resident day, and once again you can see reflected the increase in the Greenhouse of the CNA, or the Shabaz as it is known in Greenhouse. You can see also the Licensed Nurse is a little bit more in the Greenhouse home, but you see that there is actually less time per resident day, less hours per resident day. Again, that expensive administrative clinical lead time in Green, you can see much more in a traditional nursing home – the layers, the hierarchy and such that are required to make a traditional home work. That’s costly, it does come at a cost, so you can see getting more of the direct care staff to the resident is what’s so important. Back to you, Jamie.
[Jamie]
I’m going to just provide a couple of slides here and wrap us up on strategies that we’ve worked with Susan and her team and our clients on how to implement the Green House offering on an organization’s campuses. One of the things that I kind of alluded to at the beginning is, you know, somebody might come in and say, “we want to make sure that what we implement needs to be a profitable or worthwhile endeavor”, which is obviously a very important statement. However, one of the things we always ask our clients is: How do you see the Green House and just in general, the skilled nursing environment on your campus functioning? We typically try to get them to commit to an avenue. There’s two avenues that you can look at. You can either have a Green House project on your campus that supports your entire campus, and the profitability of of the homes might be either close to a break-even level or slightly losing money. If you think about how is your existing school nursing currently functioning on the campus? In many cases that’s exactly how they’re already functioning, so are you trying to offer a Green House product on your campus to help one provide that much better quality of life, a better environment and a better working situation for many individuals that Susan just outlined for us? You have that ability to provide and use that from a marketability standpoint so that if you have a portfolio or a campus that has many care levels on it, are you looking at that when a person tours your campus, they might be coming in and touring an assisted living environment or an independent living environment? You almost look at the Green House in a sense to say, I also want to showcase this is how we have our skilled nursing product as well. I find many providers will often use that as something to brag about and boast about that. They have that environment on their campus to offer their residents should they need that level of care. Whereas if you play the opposite many times, if someone has multiple care levels on their campus and the resident were to come in and look for independent living, if you have an old dated, skilled nursing environment, you’re probably avoiding it from a marketing standpoint, not touring that resident through that. That’s one certain avenue: do you want to use the Greenhouses to support your existing portfolio or a campus?
The Second Avenue is: you’re going to actually look at this to say, no, this needs to be a profit center and I want to I want to have my Greenhouses generate profitability that can support itself on a standalone basis. If that’s the case, there needs to be an unbelievable amount of discipline related to how you market those products and the type of payers that you ultimately have moving into that care environment. One of the examples I wanted to walk us through is an example we went through with a client. Susan and her team were involved in this as well. What I kind of outlined is at a very high level, where they started( and this was actually happening right at the onset of Covid). What they had is they were currently operating a 175 bed, 5-storey skilled nursing building and they knew that that environment that they were offering residents was considerably shrinking (they were having less and less people choosing to live there), and they were having a harder time providing the quality of life that they wanted to for many of their residents. On this first chart in the top right is what their existing unit occupancy was and the number of residents that resided in the different payer types. They had about 150 residents that lived in that existing building that they offered, and about 106 of those residents were Medicaid payers. They wanted to say, “we know this is not a sustainable environment, we want to start to offer more of a Green house home on our campus.” They had an assisted living that was down the road from their from their skilled nursing environment so they looked at a master plan where they built five different Greenhouses that surrounded the campus, and then they were also going to add an Independent in a memory care building that would attach into their existing assisted living. What they asked us to look at, though, is they wanted to see: if we just built those Green homes, how would those financially work and what do we need to do in order to get those financially to be above a 1.2? Their their target was to be either at or right about a. 1.2 debt service-coverage ratio. The sensitivity that we started to outline for them and provide them those numbers is to show them a couple of things. What we did is we essentially started demonstrating to them the ability or the impact that their Medicaid population had on their organization. We created a matrix and we showed them that these top percentages represented the percentage of residents that would be Medicaid payers, and then the bottom numbers kind of along the middle of this table represent the number of residents that would either be a Medicaid, or a private payer, or a Medicare resident that would reside in these five different Green homes that they were planning to build. Then we played with the different interest rates that they had at the time, where rates were much lower, they were actually closer for them. They probably could have gotten a rate at about 3.75%, but we were keeping them conservative and running all the analysis for them at about a 4.5% interest rate. The baseline that they looked at is if they still had 45% Medicaid population, their debt coverage ratio would be only a 0.88% Coverage. What we looked at is that if you’re able to maintain and be disciplined and reduce your payer mix from 45 to 35 (which essentially takes your Medicaid population down to about 25 residents), you’d be very close to achieving that 1.2 coverage, and those six Green homes would be able to operate on their own. The conversation with them started to be around what is the right payer mix that they ultimately wanted to provide to the community? And did they feel this was a nonprofit? Did they feel it? It contradicted their mission at all if they were to be so diligent and drive their Medicaid population down.
Some of the times that’s the conversation that providers are grappling with is: where do we feel like we’re almost a mission driven if they’re nonprofit? What do they feel like they should be offering or allowing from a population? They had no problem attracting and getting residents to move in and pay a private pay rate in this. In this scenario, the highest number we were assuming is that they would have 36 private payers and 11 Medicare, which is essentially already what they were achieving previously in an environment that was drastically worse than what they were proposing to provide to the residents. This exercise was something that was eye-opening enough for them to realize that the way they decided to operate their campus function really was a major driver, and this is something that our organization needs to address and tackle very early on because essentially saying that I’m going to provide a Greenhouse on our campus, but then thinking, you’re going to operate it from a payer mix standpoint identically to how you’re operating your existing and skilled environment – you need to realize that the outcome will be the same. Just because you offer financially, just because you offer a different housing environment, does it mean that your finances are magically going to improve if you have the same payer mix? Those are things that are drastically important to understand as you go into this.
The other piece that we had a long conversation about goes back to a little bit of the marketability. Personally, I thought we were a little conservative in this analysis because they were they were able to achieve, as I mentioned, 33 private pay residents in this existing environment that they had (that again, which was really not a great setting). That competition they had in the market was also extremely old and dated, so we started to ask them, Don’t you feel that you’ll be able to start to capture additional market share in the market and you start to look at the marketability of one? Will people be more attracted to live in these new environments and to if you are more attractive, are you able to charge slightly more from a private pay standpoint? A lot of cases, the hands-down answer would all almost all the time be: yes. The reason being is if you look at what your traditional skilled nursing environment is, I mean, think about this client example that we’re giving where you have hundreds of residents that would have to come down an elevator and eat in one single dining room. 150 residents essentially doing that in their campus versus a Greenhouse where each house has their own dining and kitchen and in their care staff in their shabaz that Susan just walked us through, are cooking the meals in front of the resident sitting with them, eating with them and providing those meals with them? They all have private rooms. They have the quality that they have, that they are able to offer a resident. Irving used an example of Would you live in a Hilton that’s been hasn’t been renovated or 40, 50 years old?
Our argument always is if you have two different hotels that you’re trying to choose between and someone were to say, you can choose between a Red Roof Inn or a Ritz Carlton, and the Ritz-Carlton is priced at the exact same price as a Red Roof Inn, what do you think most of your consumers are going to choose? Without a doubt, everyone’s going to choose a Ritz Carlton. Then the argument could be: what’s the appropriate premium that you’re going to charge on a Greenhouse private pay room because it is one of the best products that’s being offered in that market and then seeing how those also impact your financials. Those are conversations that just because you’re offering a skilled environment, you’re offering a far superior environment and a lot of cases to what your existing competition is. Knowing your market and pricing that appropriately is also a very critical component when you’re working with with repositioning and campus this way.
[Irving]
I think both you and Susan did exactly what we’d hoped. You’ve framed the issues extremely well and I know that there are lots of questions. I’ve got at least eight of them scribbled down here, but we we obviously have some in the Q&A box.
QUESTIONS
[Romilly]
The first question is: The slide on staffing and cost shifting where you use 60 elders – how is that physical environment designed?
[Susan]
The physical environment where it could be five homes of 12 elders in each home, or six homes of 10 elders in each home. But these are separate greenhouse homes, autonomously functioning homes. It was looking solely at the FTEs that would be essential to staffing 60 elders in Greenhouse homes.
[Romilly]
Thank you. How many greenhouse project terms are there at the moment?
[Susan]
We have 362 Greenhouse homes in 32 states, and I think we went into the pandemic with 298 homes. So that tells you kind of even through the pandemic, that there were green households that were able to open and, you know, went through that construction phase and the whole nine yards and got their homes opened and shelters moved in. It’s pretty exciting to see that happen.
[Romilly]
Any plans for international Greenhouses?
[Susan]
You know, it’s really interesting with the onslaught of COVID because it was not confined to the U.S. as we all know, it’s a global economy, if you will. We have been approached by several different countries, a lot in Canada. We’ve certainly been having conversations with some in the UK, Ireland being the most recent. We’ve had some in Africa, Australia and that we’ve been talking to pretty seriously. Oh, Israel as well.
[Irving]
It’s a model that just makes so much sense, and as we said at the top of the discussion, Jamie framed the issue, I think very well. The question is how to make the numbers work. There are lots of infrastructure and regulatory and administrative assumptions that those who are familiar with the business make it just part of how we think about things and the assumptions about the universal worker. The next the biggest topic has to do with manpower, labor, workforce issues in long term care. The question I have for Susan and possibly for Jamie: based on your experience, what’s the profile of the typical universal worker? I can’t get used to saying that other word. So forgive me because universal worker who needs to be a jack of all trades? What’s a typical profile? How difficult or easy is it to recruit them, retain them? And what do you have to pay them?
[Susan]
I’ve heard people saying you don’t want experienced people – we’ll hire for attitude and we’ll train them and give them the skills that they need and others say, Oh no, if you’re doing a universal work or you want them to have a core skill set that is about how to provide care. What I have heard and I thought one of the wisest statements from a leader of Greenhouse Holmes, she said, it’s really about finding people who have a heart. No one would have experienced working as a team. She talks to the interview process. Tell me about the teams you’ve been a part of because it’s so important to really know how to work together and the dynamics around teamwork is are so important. That’s one of the things that she suggested is pretty critical. I think to your point about what do you have to pay them? We recommend in our proforma that you do a 10 percent bump to what you’re paying a traditional see. And we did a wage survey in 2017, I believe it was, where we found some that in a unionized facility, they were only able to do a 3% increase, they said. We were at the top of our market and it was the rate we negotiated with the union and the highest was about a 35% increase. In that case, they said we were at the bottom and we did a competitive wage analysis of who’s paying what in our neck of the woods. We said we’ve got to increase and we believe because of the additional education and training that it’s worth it. We’re asking them to be more, do more and give them the education to do it.
[Irving]
That’s a good, principled response. I know there’s a lot of granularity, an awful lot of devils in those in those details. For Jamie, one of the things that struck me about Jamie’s presentation was the assumption that the requirement that operators, owners, investors, that we look at our assets differently, that we consider not only the current built environment, but what’s possible. The question for you that haunts my reveries is: how do we get access? How do we get an operation that’s running at 0.8 percent margin? How do we get an operation who can’t necessarily assume more debt? How do we get access to capital to make these investments in the physical property in the campus?
[Jamie]
I would address that from a very global perspective across the industry, because I do think that the organizations who have not invested in our single site and are functioning at a zero percent margin, essentially, might not have the ability to get access to that capital to be totally transparent if they don’t have cash reserves or investments in a single site, and they likely probably don’t have. I mean, hopefully you don’t have a lot of debt already on their books, the ability for them to totally reposition without almost essentially saying we’re going to go entirely private pay or Medicare or sources unless they make that decision. The ability for them to fund those debt amounts that they’re going to have to take on could be very difficult. So a single-site provider might struggle. The organizations that are built, that have some capacity to either liquidate portions of assets that they have and use those funds to help fund some of the cash requirement for a project and then go out and either access the fixed rate bond market or you could do traditional bank loans. We have a project right now that is going through a skilled nursing repositioning where they’re not necessarily doing the Green House, but they’re introducing the household neighborhood model to four different neighborhoods. If they’re able to kind of chop up their existing environment to and they’re converting them all to private wing, they’re accessing capital through the United States Department of Agriculture (USDA). Their capital access that they got was a 2.25 loan for 35 years, that one of the best terms out there. It’s a bit of a process to go through, to work with USDA to get those funds, but there’s avenues out there. I think you need to really kind of be creative and work with either a consultant or a banker to say there’s not one size fits all. You might have a project that could be dead with one option, but totally viable with another. Exploring what’s out there is is something that we would always encourage because it’s kind of two big pieces you got to juggle. You’ve got to juggle the cost of doing the project and what that brings from a debt perspective and then truly how you’re going to operate that campus. The ability for those two to kind of marry each other and pay for pay for one another is that kind of dance and puzzle that you end up going through.
[Irving]
That’s a very good answer, and I do know that USDA has some very significant advantages so I’m sure that other people will be interested in that as well.
The one question that I’d like to put for both Susan and Jamie has to do with the acceptance of the limitations associated with greenhouse. So the consumers that you showed and the residents that typically occupy Greenhouse are not the advanced neurologically disabled individual who very often are the individual with severe or second stage Alzheimer’s related disorder. What are the limitations associated with? Who can benefit? Who’s able to live in one of these small houses is a greenhouse project.
[Susan]
The research that I use for the total time hours per resident day in that same study, they found that there was no difference in acuity level, none whatsoever between greenhouses and their traditional counterparts that they compared them with. These are licensed and skilled nursing, and so this is home for life. It’s one of the trademark requirements at its home for life. In Boston, they care for people that are actually on ventilators. And we did research where it showed 85% of those living in Greenhouse homes were living with mild to severe cognitive impairment. I think they don’t look to be having some of the limitations you described, but there’s something about normalizing our programs in our environments and the impact that it has on the person. When you put someone, if you don’t put them in their street clothes, if you’re not getting them outside, if you’re keeping them in their room and I can tell you they weren’t measuring antipsychotics during the pandemic, but I guarantee you if you put somebody living with cognitive impairment in the room that they share with somebody else and said, you can’t go anywhere. I’m pretty sure that there is antipsychotic usage that went up, but in a Greenhouse honoring the natural rhythm, you’re able to really meet those unmet needs or what we might call the behavioral expressions, that result is because those needs weren’t met.
[Irving]
It continues to be a fascinating model and a challenge for those of us who have been in the business for a long time to wrap our heads around in the particulars in general. Of course, it’s very appealing, very attractive model. I want to thank you, Susan, for your pioneering work in this regard. I want to thank you, Jamie, for making us look at these numbers and that these fiscal issues in a different light. I want to thank the folks who showed up and took the time to participate.
Susan Ryan | Senior Director | The GREEN HOUSE Project
sryan@thegreenhouseproject.org
Jamie Timoteo, MBA | Principal | Plante Moran Living Forward
Jamie.Timoteo@plantemoran.com
Resources
- Zimmerman et al_Nontraditional Small House Nursing Homes and COVID.
- Williams, B. Failure to Thrive? Long-Term Care’s Tenuous Long-Term Future.
See: https://scholarship.shu.edu/shlj/vol43/iss2/3/ - True, S. et al. COVID-19 and Workers at Risk: Examining the Long-Term Care Workforce.
- Stackpole, I. Bridging the Divide: Transitions to Cross-Continuum Collaborations in Healthcare.
See: https://stackpoleassociates.com/transitions-cross-continuum-collaborations-healthcare - Adoption factors associated with electronic health record: www.ncbi.nlm.nih.gov › pmc › articles › PMC4316426
- Who Cares? The pandemic shows the urgency of reforming care for the elderly. The Economist.
- Jan 28, 2015 – Long-term care (LTC) facilities (as defined by the ARRA) are facility types excluded from the incentives including: skilled nursing homes, assisted … also a source of statistical inference when ‘meaningful use’ is assessed. See: Final Report of NH Commission Public Release Case.pdf
- Coronavirus Commission on Safety and Quality in Nursing Homes. September 2020.
Stackpole & Associates is a marketing, research & strategy consulting firm focused on healthcare and seniors’ services markets. Irving can be reached directly at istackpole@stackpoleassociates.com.